A big thanks to guest blogger Cyndi Laurenti for her research on how telemedicine and telesurgery are positively affecting the developing world. Cyndi recently graduated with a degree in International Relations and is interested in how public policy affects all spheres of life. She can be reached at laurenticy@gmail.com.
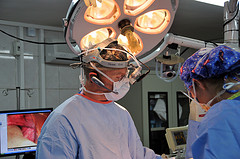 Videoconferencing has provided an answer to many problems the medical community faces. With the world population growing rapidly and limited medical resources available, this new technology offers the capability of stretching valuable resources to better meet growing patient demands worldwide. Not only has it been a way for doctors to implement cutting-edge technology to their processes, it has also been a way for non-profits to seek social impact in an innovative fashion. For example, disaster response specialist, Randy Roberson, has developed a portable solar-powered telemedicine backpack that is able to provide humanitarian relief workers with a direct video link to a doctor even in the most unpredictable environments by using satellite Internet technology with VSee, a low-bandwidth optimized videoconferencing technology.
Videoconferencing has provided an answer to many problems the medical community faces. With the world population growing rapidly and limited medical resources available, this new technology offers the capability of stretching valuable resources to better meet growing patient demands worldwide. Not only has it been a way for doctors to implement cutting-edge technology to their processes, it has also been a way for non-profits to seek social impact in an innovative fashion. For example, disaster response specialist, Randy Roberson, has developed a portable solar-powered telemedicine backpack that is able to provide humanitarian relief workers with a direct video link to a doctor even in the most unpredictable environments by using satellite Internet technology with VSee, a low-bandwidth optimized videoconferencing technology.
According to Public Administration, social innovators willserve as enablers and facilitators in the construction of institutions of social institutions. Having the ability to connect medical centers from across the world is just the beginning of such an institution. For example this tool transfers expert information from seasoned surgeons to physicians in developing countries who would not otherwise be qualified to complete many surgeries, giving patients access to specialized medical care not usually available to them.
The Medical Missions for Children GTTN
This network uses teleconferencing technology to connect U.S. mentoring medical professionals with physicians from third-world countries for the purpose of demonstrating surgery techniques. In emergency situations, an inexperienced doctor practicing in a remote area can be coached through a delicate procedure, relying on an expert in the field. This organization serves 40 countries worldwide utilizing video telehealth sessions to provide necessary treatment to people who would otherwise be forced to go without care, or to settle for less than optimal care solutions. This valuable program helps 1200 children annually.
Telesurgery and Rehabilitation Success
A medical team working out of Johns Hopkins University School of Medicine uses videoconferencing provide speech therapy to patients in Nicaragua suffering with a cleft palate. Dr. Patrick Byrne uses WebEx technology to follow up with much needed speech therapy to teach these patients how to speak after the operation. The results have been remarkable with many of the children finally able to communicate with their family and in school.
Telesurgery has been used successfully in Irag and Afghanistan to operate on U.S. soldiers. By using a high resolution camera to reproduce the operating table for the remote surgeon expert to see, a local physician can be instructed by the expert about the details of the operation. For example, the training physician can indicate where the local doctor should cut by circling the exact location on the patient via a screen they both see. LTC Dr. Sloane Guy performed a complicated surgery using this technology to save a soldier’s life in Iraq. He received instruction from Brooke Army Medical Center during the operation.
When Damaris Njeri’s life was threatened by failing kidneys, she was faced with a formidable economic and logistics challenge. As a woman of limited means who lived in Kenya, telesurgery allowed a local physician to save her life, under the direction of an expert surgeon located in Nairobi. The urological procedure was successfully performed in the local Aga Khan University Hospital.
Reflecting on the Politics of Telesurgery
Telesurgery offers a technological answer to the limited medical resources available to operate on patients in remote parts of the world. There is little doubt that this tool will remain an excellent training resource. The practical usage of “real-time” telesurgery worldwide both creates and solves certain challenges. Who will ultimately pay for these surgeries that cross the borders? Are there enough experts in the world available to handle the number of “real-time” surgeries needed? Who decides who will receive the benefit of telesurgeries and who will not? How will time delays affect the patient if something goes wrong during a telesurgery? It is obvious that the technology is in place. But politics will ultimately dictate whether developing countries will benefit from telesurgery as a realistic answer to a growing problem.
Will telesurgery benefit those lacking the resources or will it end up being another expensive technology only for those who can pay for it.
Follow us on Twitter (@VSee) and Like us on Facebook to hear about the latest from VSee!
photo credits: MC4 Army



